A corneal transplant is sometimes necessary when the corneal tissue becomes damaged due to injury, infection, or disease.
The cornea is the clear, dome-shaped front surface of the eye. Most of the refractive and focusing power of the eye is in the interface between the cornea and the air. Without a functioning cornea, you would likely see very blurred or distorted images, and in severe cases, you might only perceive light and shadows.
Fortunately, corneal transplant surgery is one of the services we offer at Eye Care Institute in Santa Rosa, California. Dr. Nina Ni specializes in this procedure and can help improve your vision if your cornea is failing.
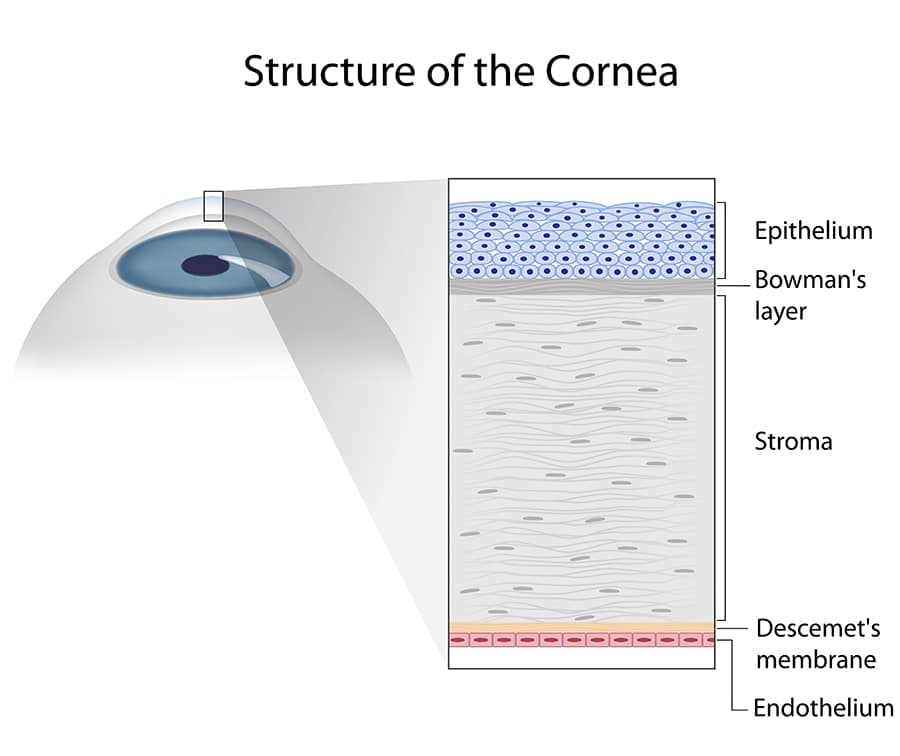
What Is a Corneal Transplant?
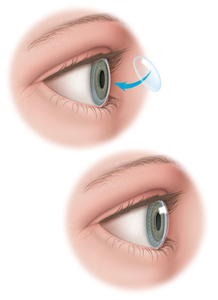
During a corneal transplant, Dr. Ni replaces damaged tissue with healthy donor tissue obtained from a local eye bank. Traditionally, a penetrating keratoplasty (PKP) would be the type of corneal transplant required to treat many corneal problems.
At ECI, we also use advanced surgical techniques to improve visual outcomes and shorten recovery time.
Corneal transplants are the most common type of transplants done in the world, with a success rate of over 90%.
Corneal Transplant
Increasingly, the cornea has been the focus of advanced laser and surgical procedures to correct vision for those with medical ocular problems. It’s also an option for those who don’t want to rely as much on glasses. Examples of these new advances in surgical procedures include:
- Descemet Stripping Endothelial Keratoplasty (DSEK): Replaces the damaged back layer of your cornea with healthy donor tissue, helping you recover faster and reducing the chances of rejection.
- Descemet Membrane Endothelial Keratoplasty (DMEK): Replaces only the very thin inner layer of your cornea for quicker vision improvement and better results.
- Deep Anterior Lamellar Keratoplasty (DALK): Replaces the front layers of your cornea while keeping the inner layer intact. This reduces the risk of rejection and treats issues affecting only the cornea's front part.
There is generally no shortage of corneas in America due to the excellent eye banks around the country. Eye banks are now supplying increasingly sophisticated pre-cut tissue for treating problems with either the front of the cornea or the posterior part of the cornea.
Conditions Most Likely to Require a Corneal Transplant
Since the cornea is the foremost part of the eye, the cornea is often a target for injury. The following conditions are a partial list of traumatic corneal problems that might require eventual corneal transplant surgeries:
- Foreign bodies in the visual axis
- Chemical injuries
- Penetrating injuries, such as industrial accidents
- Lacerations from blunt trauma
- Drying from injuries that prevent the eyelids from closing
- Endothelial dystrophy (a condition that affects the innermost layer of the cornea, leading to fluid buildup, cloudiness, and vision impairment)
- Bacterial and viral corneal infections
- Persistent corneal swelling after cataract surgery
The cornea has remarkable healing properties and copes very well with minor injuries or abrasions. Deeper scratches or injuries can result in scarring. When this occurs in the visual axis, the vision may be affected, even to the point of blindness.
Corneas with partial-thickness scars can be treated with traditional penetrating corneal transplants or, in some cases, with deep lamellar or a partial corneal transplant. The deep anterior lamellar transplants (DALK) have a quicker recovery. Patients with scarring from keratoconus or who have become unable to wear contacts to correct their keratoconus are often suitable for this meticulous and technically challenging type of corneal transplant.
What to Expect During a Corneal Transplant at Eye Care Institute
Before your surgery, we’ll give you a sedative. You’ll be awake during the procedure, but your eye will have local anesthetic, so you won’t feel anything.
In the most common type of corneal transplant, Dr. Ni cuts through the entire thickness of the abnormal or diseased cornea to remove a circular disk of tissue. To precisely make this cut, she uses a trephine that will make the circular button-sized cut.
Then, she cuts the donor cornea to fit the same size and places it in the space of the removed circle of tissue. Dr. Ni stitches this new cornea into place, and the procedure is complete.
*In some patients, full-thickness corneal transplants aren’t the best option. These procedures remove certain layers of cornea tissue, either the back or front layers, which we then replace with donor tissue.
When Can You See Again After a Corneal Transplant?
Dr. Ni will have an eye patch over the eye with the transplant. This will be in place for one to two days; we’ll remove it when you return for your checkup to see how your eye is healing. Your initial vision will likely be worse than it was before your surgery, but this is only temporary. Still, it can take months for your eye with the transplant to fully improve.
Because you only have surgery on one eye, your other eye is unaffected. That enables you to see normally from that eye, even as your other eye heals and improves.
Why Choose Eye Care Institute?
Our specialists at Eye Care Institute bring a blend of advanced training and a patient-first philosophy. Dr. Nina Ni is one of our highly skilled, board-certified ophthalmologists with a compassionate approach to patient care. Dr. Ni specializes in corneal surgery, cataract surgery, and comprehensive ophthalmology. Her extensive training and experience allow her to provide top-tier care for every patient.
But we pride ourselves on more than our clinical skills; we’re committed to making each patient feel valued and heard. Our compassionate approach is what truly sets us apart. From the moment you step into our clinic, you will experience a warm, welcoming environment where your concerns are our priority.
Experience the difference at ECI, where your vision and well-being are at the heart of everything we do.
Frequently Asked Questions
How Should I Prepare for a Corneal Transplant Surgery?
Getting ready for a corneal transplant involves a few key steps to ensure everything goes smoothly. Here’s what you should do:
- Have a Comprehensive Eye Exam: Dr. Ni will thoroughly check your eye health to ensure you’re a good candidate for the surgery.
- Discuss Your Medical History: Be open about any medications you’re taking and your overall medical history with Dr. Ni. This helps her plan the best approach for your surgery.
- Follow Medication Instructions: Before the surgery, you might need to stop taking certain medications, like blood thinners. The doctor will give you specific instructions on what to do.
- Arrange Transportation: Since you won’t be able to drive home after the procedure, make sure you have someone who can take you home safely.
How Long Does a Transplant Procedure Take?
These transplants take from one to two hours, depending on whether they are full thickness or layer replacements.
How Long Does a Transplant Last?
There is no set timeframe for how long these transplants will last. Research has shown that transplanted corneal tissue can last 10-20 years or more. It can improve your vision to between 20/20 and 20/40 with corrective contact lenses or glasses.
What Is Recovery Like After a Corneal Transplant at Eye Care Institute?
Total corneal transplants can require recovery times of a year or longer. Initially, your vision will be blurry for the first few months. It can be worse than before your surgery, which can be disconcerting. Your eye simply needs to get accustomed to your new cornea. Generally, DMEK and DSEK patients achieve good vision more quickly.
Your vision will improve, and you can return to your normal daily activities. You’ll have to avoid heavy lifting and strenuous exercise for several weeks to keep from elevating the blood pressure in your face and eyes. Depending on their occupation, most patients can return to work within a week after these surgeries.
You’ll use prescription steroid eye drops for several months after surgery to help your body accept the new corneal graft. Other medications will help control swelling, discomfort, and the possibility of infection. You’ll wear eyeglasses or an eye shield at all times to keep from inadvertently bumping your eye.
If you have stitches, we’ll remove them anywhere from three to 17 months after surgery, depending on your healing rate. We can make adjustments here to help reduce the amount of astigmatism you experience.
How Long After My Corneal Transplant Will I Be Able to Drive Again?
This depends upon your vision quality in your other eye. Some patients have good vision quickly and can drive only a few days after surgery. However, we will likely advise you to wait a little longer.
Who Is a Candidate for Corneal Transplant Surgery?
Candidates for corneal transplant surgery typically include individuals whose vision has been significantly impaired due to damage or disease affecting the cornea.
You’ll be evaluated based on the severity of your condition, your overall eye health, and your likelihood of benefiting from the procedure. Good candidates are typically those who have not responded well to other treatments and whose corneal condition several impacts their quality of life.
What Is the Long-Term Outlook for Patients After a Corneal Transplant?
The long-term outlook for corneal transplant patients is pretty encouraging, with many people seeing significant improvements in their vision. However, keeping your new cornea healthy requires some ongoing care. You'll need to go to regular follow-up appointments, stick to your prescribed medications, and be careful to protect your eye from injury.
The success and longevity of your transplant can depend on several factors, like the underlying condition that led to the transplant, the type of procedure you had, and how well you follow post-operative care instructions.
What Are the Risks Involved With a Corneal Transplant?
These are relatively safe procedures, but there are some risks. The biggest risk with corneal transplants is that your body will reject the donor cornea. This occurs in nearly a third of corneal transplant patients. It occurs when your body believes the new tissue is a foreign body and attacks it.
However, if you recognize the warning signs of tissue rejection, you can better prevent graft failure. To remember what to look for, use the acronym RSVP:
- Redness
- Extreme sensitivity to light
- Decreased vision
- Pain
The possibility of rejection can last for years after your surgery; that’s why you’ll use steroid drops. If we can detect those signs of rejection early, the graft can still be successful around 90 percent of the time.
Other possible risks include eye infection, increased risk of cataracts, increased pressure within the eyeball (glaucoma), problems with stitches, and cornea swelling.
Book Your Corneal Transplant Consultation in Santa Rosa!
For more information on corneal transplants or to schedule an appointment today with Eye Care Institute, call us today at 707.546.9800 or contact us online. Our practice serves Santa Rosa and the surrounding areas of California.